The Uncomplicated Truth About Diabetic Retinopathy (And How to Protect Your Vision)
If you have diabetes, one of the most important parts of your health that often gets overlooked is your vision.
Diabetic retinopathy is one of the leading causes of blindness in working-age adults—but the reassuring part is this:
It is often preventable, and treatable if detected early.
Prefer a quick explanation? Watch this short video where I explain diabetic retinopathy and how to protect your vision:
If you have diabetes and are unsure about your eye health, a simple retinal check can detect early changes—even before symptoms appear.
What is diabetic retinopathy?
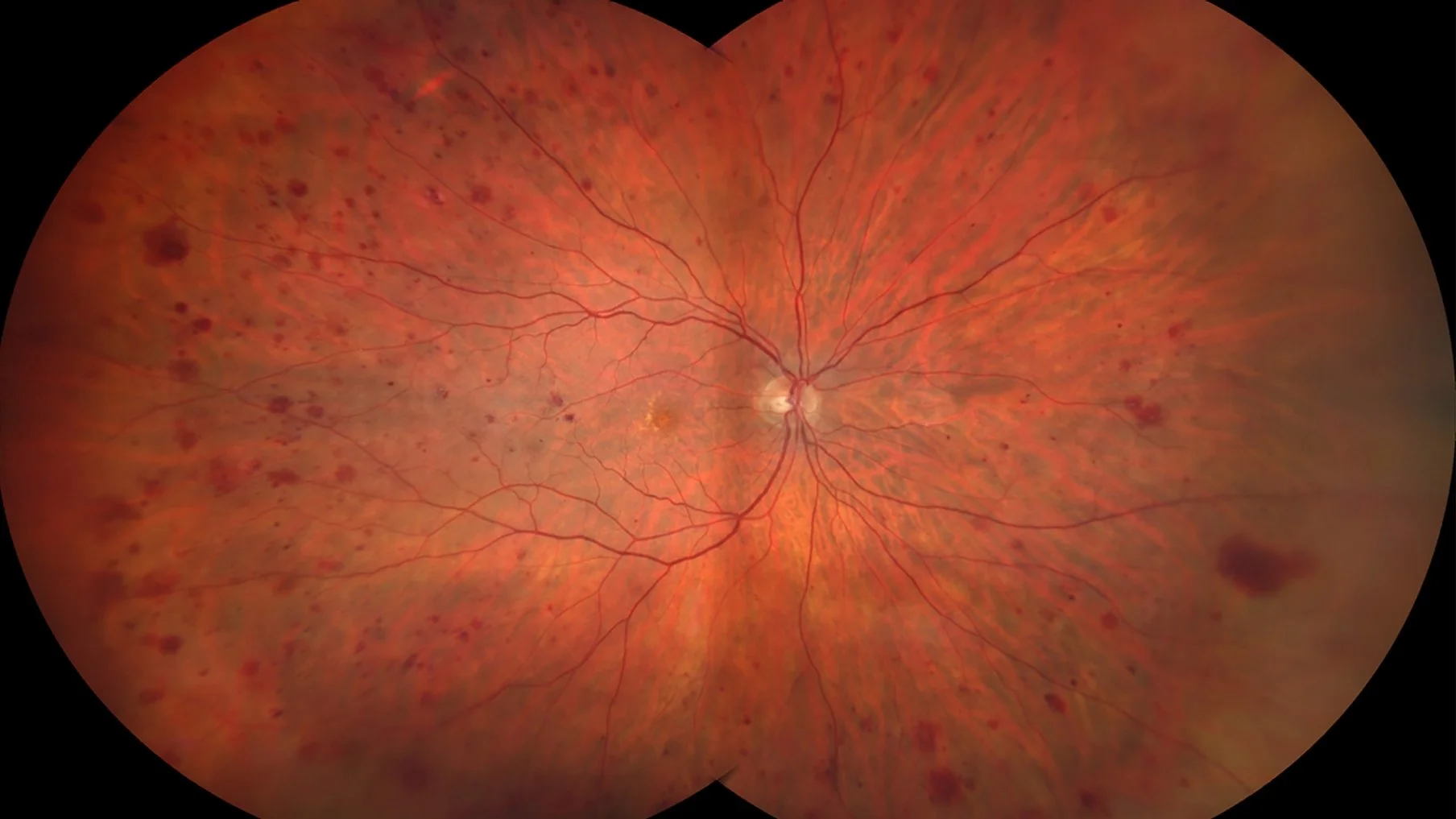
Diabetic retinopathy is a complication of diabetes that affects the retina, the light-sensitive layer at the back of your eye that allows you to see. Over time, high blood sugar levels can damage the small blood vessels in the retina. These vessels may:
weaken
leak fluid or blood
or become blocked
In more advanced stages, the eye may even grow abnormal new blood vessels, which can cause serious damage.
The two main stages (simplified)
1. Early stage (non-proliferative diabetic retinopathy)
This is the most common and earliest stage.
Blood vessels become weak and leaky
Small haemorrhages or fluid leakage may occur
Vision is often still normal
👉 This is why many patients don’t realise they have it.
2. Advanced stage (proliferative diabetic retinopathy)
This is the more serious stage.
The retina becomes starved of oxygen
Fragile, abnormal blood vessels grow
These can bleed, scar, and even cause retinal detachment
👉 This stage carries a high risk of permanent vision loss if untreated.
What is diabetic maculopathy?
This is a related condition where fluid leaks into the macula (the central part of the retina responsible for sharp vision). It can occur at any stage and typically causes:
blurred central vision
distortion (straight lines appearing wavy)
What are the symptoms?
One of the most important things to understand:
👉 Early diabetic retinopathy has no symptoms.
As it progresses, you may notice:
Blurred vision
Floaters (small dark spots or shapes)
Dark patches in your vision
Distorted or wavy lines
When should you be concerned?
You should seek urgent eye assessment if you notice:
Sudden worsening of vision
A significant increase in floaters
Dark shadows or missing areas in your vision
Who is at risk?
The biggest factor is how well your diabetes is controlled.
Key risk factors include:
High HbA1c levels
Long duration of diabetes
High blood pressure
High cholesterol
Kidney disease
Smoking
Pregnancy
A useful benchmark:
👉 Keeping your HbA1c below 7% significantly reduces your risk
In fact, studies have shown that even a 1% reduction in HbA1c can reduce complications by ~30–35%.
How is diabetic retinopathy detected?
Because early stages are silent, screening is essential. Detection usually involves:
Retinal photography
Dilated eye examination
OCT scans (to detect swelling or fluid)
Occasionally, dye tests to assess blood flow
How is diabetic retinopathy treated?
Treatment depends on the stage:
Early stages
Often no direct eye treatment is needed
Focus is on controlling:
blood sugar
blood pressure
cholesterol
More advanced stages
Treatment may include:
Laser therapy to stabilise the retina
Intravitreal injections to reduce leakage and abnormal vessel growth
These treatments are highly effective at:
preventing further damage
preserving vision
The most important thing you can do
If there’s one key takeaway, it’s this:
👉 Diabetic retinopathy is often silent - but not harmless.
The single most effective step you can take is:
Regular annual eye screening, even if your vision feels completely normal
A practical approach to protecting your vision
Keep HbA1c under good control
Manage blood pressure and cholesterol
Avoid smoking
Attend regular diabetic reviews
Have your eyes checked at least once a year
Final thoughts
In clinic, one of the most common things I hear is:
“My vision is fine, so I thought everything was okay.”
Unfortunately, diabetic retinopathy doesn’t work that way. By the time symptoms appear, the disease is often already more advanced. The good news is that with early detection and proper management, we can prevent the vast majority of serious vision loss.
If you have diabetes and haven’t had a recent eye check
It may be worth arranging one—even if everything feels normal. Early reassurance is always better than late treatment.
Watch the full explanation here if you prefer video → https://www.youtube.com/watch?v=SIVMOK3ZCjw